1. Introduction to Amyloidosis Cutis Dyschromica
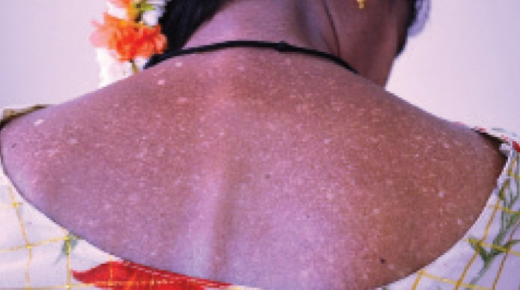
Amyloidosis cutis dyschromica (ACD) is a rare skin disorder characterized by abnormal deposits of amyloid protein in the skin, resulting in distinctive pigmentary changes.
2. Understanding Amyloidosis
Amyloidosis refers to a group of conditions characterized by the abnormal accumulation of amyloid protein in various organs and tissues, leading to organ dysfunction.
3. Dyschromic Skin Lesions
The hallmark feature of ACD is the presence of dyschromic skin lesions, which typically manifest as hypo- and hyperpigmented patches on the skin.
4. Onset and Progression
ACD usually presents in childhood or adolescence and may progressively worsen over time, although the course of the disease can vary among individuals.
5. Etiology and Pathogenesis
The exact cause of ACD remains unknown, but genetic factors may play a role in predisposing individuals to the condition. Abnormalities in the production and deposition of amyloid protein are thought to contribute to the development of skin lesions.
6. Clinical Presentation
Skin lesions in ACD are typically asymptomatic but may cause cosmetic concerns due to their distinctive appearance. Lesions are usually found on the trunk, extremities, and face.
7. Differential Diagnosis
ACD must be differentiated from other pigmentary disorders, such as vitiligo, post-inflammatory hyperpigmentation, and other forms of amyloidosis, to ensure accurate diagnosis and appropriate management.
8. Diagnosis
Diagnosis of ACD is typically based on clinical evaluation, skin biopsy, and histopathological examination, which reveal characteristic findings of amyloid deposits within the skin.
9. Management and Treatment
There is no specific treatment for ACD, and management primarily focuses on cosmetic camouflage and sun protection to minimize the appearance of skin lesions and prevent further pigmentary changes.
10. Psychological Impact
Living with ACD can have a psychological impact on affected individuals, leading to feelings of self-consciousness and decreased quality of life. Counseling and support groups may be beneficial in addressing these concerns.
11. Genetic Counseling
Genetic counseling may be offered to individuals with ACD and their families to discuss the inheritance pattern of the condition and the risk of passing it on to future generations.
12. Research and Advances
Ongoing research into the underlying mechanisms of ACD may lead to the development of targeted therapies aimed at preventing or reversing the deposition of amyloid protein in the skin.
13. Prognosis
The prognosis for ACD is generally favorable, as the condition does not typically affect overall health or life expectancy. However, the cosmetic appearance of skin lesions may impact quality of life for some individuals.
14. Education and Awareness
Raising awareness about ACD among healthcare professionals and the general public is essential for early recognition, accurate diagnosis, and appropriate management of the condition.
15. Supportive Care
Providing supportive care and resources for affected individuals and their families, such as access to dermatologists, genetic counselors, and support groups, can help improve coping and adjustment to living with ACD.
16. Lifestyle Modifications
Lifestyle modifications, such as avoiding sun exposure and using sunscreen regularly, can help minimize pigmentary changes and protect the skin from further damage in individuals with ACD.
17. Coping Strategies
Developing coping strategies, such as positive self-talk, seeking social support, and engaging in enjoyable activities, can help individuals with ACD navigate the emotional challenges associated with the condition.
18. Empowerment Through Knowledge
Empowering individuals with ACD with knowledge about their condition and available resources can help them advocate for their healthcare needs and make informed decisions about their care.
19. Public Advocacy
Advocating for increased research funding and access to healthcare services for individuals with rare skin disorders like ACD can help improve outcomes and quality of life for affected individuals.
20. Promoting Inclusivity
Promoting inclusivity and acceptance of individuals with visible differences, including those with ACD, can help reduce stigma and foster a more supportive and understanding society.
21. Holistic Approach to Care
Adopting a holistic approach to care that addresses the physical, emotional, and psychosocial needs of individuals with ACD is essential for promoting overall well-being and quality of life.
22. Collaboration Among Healthcare Providers
Collaboration among dermatologists, geneticists, psychologists, and other healthcare providers is crucial for delivering comprehensive care to individuals with ACD and addressing the multifaceted aspects of the condition.
23. Family Support
Providing support and resources for families affected by ACD, including education about the condition and available support services, can help facilitate coping and adaptation to the challenges of living with the condition.
24. Future Directions
Continued research into the pathogenesis of ACD and the development of novel therapeutic approaches hold promise for improving outcomes and quality of life for individuals affected by this rare skin disorder.
25. Conclusion: Moving Forward with Hope
In conclusion, while living with ACD may present challenges, ongoing research, education, and support initiatives offer hope for improved understanding, management, and quality of life for affected individuals and their families.